Our Services
Personalized Fetal Care for Every Stage of Pregnancy
Comprehensive fetal scans, advanced prenatal diagnostics, and expert monitoring to support healthy fetal development and safe pregnancy outcomes.
Fetal Scans and Pregnancy Care
We provide a range of fetal scans and prenatal diagnostic services to monitor the growth and development of your baby throughout pregnancy. Our advanced imaging helps detect any abnormalities at an early stage and supports timely medical care. These services assist doctors in managing both routine and high-risk pregnancies. Early evaluation ensures better planning for delivery and improved outcomes for mother and baby.

Basic scans
Basic Fetal Scans We Offer
Early pregnancy / Viability scan (5-10 weeks pregnancy)
This is the first scan done in early pregnancy between 5-10 weeks pregnancy . This is to confirm the pregnancy, see if it is normally located in the uterus , are there any complications , is it developing or is it a miscarriage, is it single or twins ? This is usually a transvaginal scan. It is very important if patients have problems like stomach pain or bleeding in the early stages.
Nuchal Translucency (NT) scan / First trimester screening (11-14 weeks pregnancy)
It is done between 11-14 weeks pregnancy strictly . It is recommended for all patients. It is done to assess the risks in pregnancy for the baby and the mother . It is done to assess the risks for the baby having common chromosomal abnormalities , having growth problems in later stages and also checks the structures and development of the parts and organs of the fetus at an early stage. If there are major abnormalities in development they get detected early. For the mother , it helps assess risk of having preterm delivery, developing high blood pressure later in pregnancy, or having problems with blood supply to the baby. This is done in Nest fetal medicine centre as per the strict Fetal medicine Foundation , UK protocols and certification , both for the scan and the risk assessment calculations to ensure reliable reports. Only when standards are followed is the risk calculation valid. Very strict guidelines and audits are followed. Since the fetus is very small ( about the size of your finger) , unless detailed and standard examination is done it is not possible to detect abnormalities at this stage . In NFMC we always do a complete risk assessment for all the possible conditions and a comprehensive report is issued so that preventive treatment can be started from very early in pregnancy.
Anomaly scan / TIFFA scans (18-22 weeks pregnancy)
This is done between 18-22 weeks pregnancy . This is the most important and most detailed scan. The scan is mainly focused on examining the development of the baby completely from head to toe and make sure there is no abnormality in the structures. If it is done too early few structures may not be developed and if done too late even if there are abnormalities we may not be able to do anything about it. This is a very specialised scan like the NT scan and needs expertise , good machine and detailed examination to make sure everything is normal. If any abnormality is found, the abnormality , why it occurs, risk of genetic problems, further tests to be done, outcomes for the fetus , what treatment can be done and risks will be explained to the parents in detail. They will be given all options and help to manage the pregnancy along with a discussion with their referring doctor. In addition to checking for structural abnormalities , risk of growth problems, genetic abnormalities , pre term delivery and issues of inadequate growth will also be checked for .
Growth scan (22-42 weeks pregnancy)
This is mainly to assess if the fetus is growing properly , movements are fine ,to check the fluid levels and the blood supply. It is also called the fetal well being scan. In patients with complications like diabetes and hypertension these are very important and done more frequently. In our practise after 28 weeks we recommend monthly growth scans. In cases where the growth is not satisfactory or the blood supply is not adequate, it is crucial to identify fetuses which are at risk to die inside the womb and to deliver them early. This a fine balance to not delivery the baby too early but not let them become sick inside the womb and requires experience and expert care.
Fetal doppler and liquor assessment
This is done between 22-42 weeks pregnancy. This does not include the assessment of the weight and the organs of the fetus , unlike what is done in the growth scan. It is done to monitor high risk fetuses in between growth scans. It is to check the amniotic fluid levels and the circulation from the mother to the baby and in the baby and identify those that are not getting enough nutrition / blood supply .
Pelvic scans (2D and 3D)
This is mainly done in Gynaecology cases and is a scan of the uterus and the ovaries and the surrounding pelvic organs. It is usually transvaginal and patient need not come in full bladder unless specifically required.
Advance scan
Advanced Fetal Scans
3D and 4D fetal scans
Done at 28-34 weeks pregnancy -3D images +growth scan / 4D video clip + growth scan. So it is usually done at the time of the growth scans . It is for the parents to see the fetus especially the face in 3D or with movements and expression which is 4D. It usually does not have any medical advantage in normal pregnancies. It has added value when there are fetal abnormalities to examine the problem and to help the parents understand the condition. It is not routinely recommended to all patients . It is possible to do these scans only if the fluid is adequate and fetus position is satisfactory . If there are structures like umbilical cord or hands in front of the face it may not be possible to get images. Similarly if the fetus is facing down or face is not seen it is not possible to do 3D or 4D. in such cases the patients may have to wait for long periods with repeated examinations or may have to come repeatedly on different days. Later in pregnancy when the space in the womb is less, it is difficult to do these scans .
Fetal echocardiography
Done between16-32 weeks . It is usually preferred to do it around 22-24 weeks when the heart of the fetus is big enough and abnormalities can be detected. It is recommended in patients who have parents , previous child or family member with congenital heart abnormalities , mothers with medical complications like diabetes or SLE, or suspicion in previous scan. It is a detailed examination of the structure and function of the heart of the fetus to rule out abnormalities like holes in the heart , abnormal valves or chambers or vessels connecting in the heart.
Fetal neurosonography
Done between 16-36 weeks, This is a very specialised examination of the fetal brain in cases where there are suspected problems. It need lot of expertise since the structure and formation is constantly changing through out pregnancy until about 2 tears after birth. This scan is to try to identify abnormalities and conditions that are evolving in the fetus. It may also be recommended in cases where there are other abnormalities or suspicion of genetic problems.
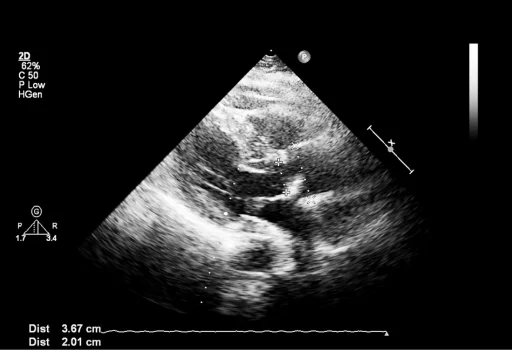
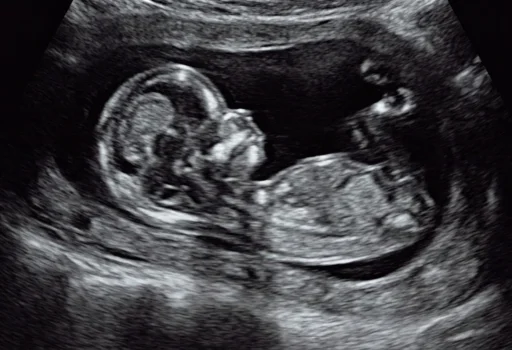

Advance procedures
Fetal Diagnostic Procedures
Fetal diagnostic procedures involve those with genetic problems in family / previous child , or tests showing risk of genetic / chromosomal problem.
- Amniocentesis – This is an invasive test to take a sample of amniotic fluid from the womb to test the cells for chromosomal or genetic problems . This includes a detailed scan and counselling before the test , genetic test and interpretation of the reports .It is most commonly doen in cases where there is high risk identified in previous scans or test , cases with abnormalities in fetal parts detected or those with genetic diseases in the family. It can be done after 16 weeks of pregnancy.
- Chorion villus sampling – This is similar to amniocentesis but is done between 11-14 weeks of pregnancy for earlier detection. Here a sample of tissue from the developing placenta is taken for testing.
- Cordocentesis – In cordocentesis a sample of fetal blood is taken for specific tests like those mentioned above.
Advance proceducers
Fetal Therapeutic Procedures
Fetal reduction procedure
It is done in higher order multiple pregnancy like twins , triplets , quadruplets , etc. IN these patients there is high risk of complications and of miscarriage or pre term delivery. So fetal reduction is done to reduce this risk and to continue the pregnancy as twins preferably. If there is abnormality of one fetus which causes the other fetus also to be at risk , the abnormal fetus can be reduced. This incudes detailed NT scan done at our unit , counselling and procedure . It is done between 11-14 weeks usually.
Intrauterine blood transfusions
This is a life saving procedure in severe fetal anaemia . In severe fetal anaemia the fetus can go into cardiac failure and die. This is prevented by doing a blood transfusion with specially prepared blood into the circulation of the foetus. It may have to be repeated few times in pregnancy in severe cases. It is most commonly done in mothers with Rh negative blood group who are sensitised.
Fetoscopic procedures
Some of these procedures are interstitial and placental Laser ablations, bipolar cord occlusion, radio frequency ablation , fetoscopic endotracheal balloon occlusion . These are extremely specialised surgical procedures done on the fetus in the womb using a fetoscope just like in laproscopic surgery. It is done in complicated monochorionic twins with problems like twin to twin transfusion (TTTS), TRAP, TAPS, selective fetal growth restriction , etc . These are very high risk pregnancies which will require close monitoring before and after procedures as the risks of complications are very high. There are no centres in our state offering all these procedures. In case of doctors enquiring about the same please facilitate a discussion directly.
Shunt procedures
This is done to put a shunt to help drain excess fluid collections like around the lungs, in the kidney or bladder of the fetus . This helps protect the fetal organs until the fetus can be delivered and treatment can be done outside.
